Posted 20 October 2004
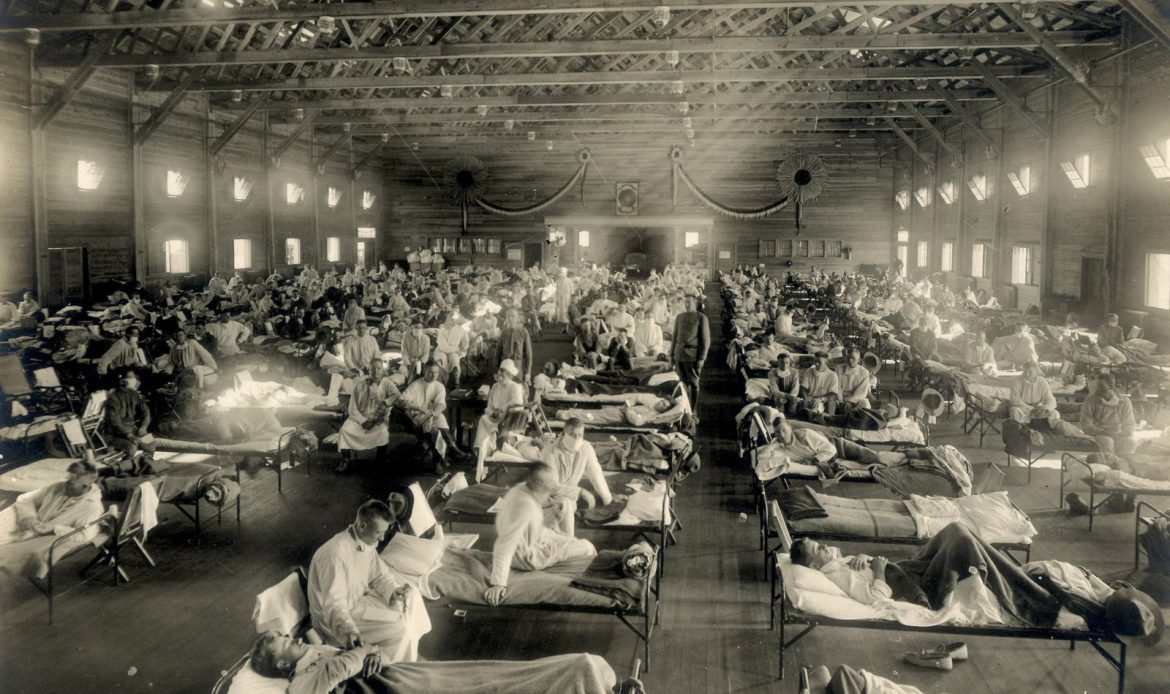
The 1918 flu virus spread across the world in three months and killed at least 40 million people. If it escaped from a lab today, the death toll could be far higher. “The potential implications of an infected lab worker – and spread beyond the lab – are terrifying,” says D. A. Henderson of the University of Pittsburgh, a leading biosecurity expert.
Yet despite the danger, researchers in the US are working with reconstructed versions of the virus at less than the maximum level of containment. Many other experts are worried about the risks. “All the virologists I have spoken to have concerns,” says Ingegerd Kallings of the Swedish Institute for Infectious Disease Control in Stockholm, who helped set laboratory safety standards for the World Health Organization.
Work on the 1918 flu virus is not the only worry. Some experiments with bird flu have also been criticised as dangerous (New Scientist print edition, 28 February 2004).
Kallings and others are calling for international discussions to resolve the issues related to such work. “It is time for influenza scientists to find a consensus on containment,” she says. John MacKenzie of the University of Queensland in Australia, who investigated how the SARS virus escaped from high-level containment labs in east Asia on three occasions after lab workers became infected, agrees. “A meeting would be beneficial.”
Gene sequencing
The researchers working on the 1918 virus say their work is vital to understand what changes make flu viruses dangerous. So far five of the 1918 flu virus’s eight genes have been sequenced, using fragments retrieved from victims of the pandemic. Several teams have added one or more of these genes to modern flu viruses, or plan to – in effect partially recreating the long-vanished pandemic virus.
The latest work was done by Yoshihiro Kawaoka at the University of Wisconsin at Madison. His team showed that adding the 1918 gene for the surface protein haemagglutinin to modern viruses made them far deadlier to mice. The researchers also found that people born after 1918 have little or no immunity.
The team started the work at the highest level of containment, BSL-4, at Canada’s National Microbiology Laboratory in Winnipeg. Then they decided the viruses were safe enough to handle at the next level down, and did the rest of the work across the border in a BSL-3Ag lab in Madison. The main difference between BSL-4 and BSL-3Ag is that precautions to ensure staff do not get infected are less stringent: while BSL-4 involves wearing fully enclosed body suits, those working at BSL-3Ag labs typically have half-suits.
Kawaoka told New Scientist that the decision to move down to BSL-3Ag was taken only after experiments at BSL-4 showed that giving mice the antiviral drug oseltamivir (Tamiflu) in advance prevented them getting sick. This means, he says, that if all lab workers take oseltamivir “they cannot become infected”.
Contradictory results
Yet this assumes that the mouse results apply to humans. And the findings have not been published. In similar experiments, Terrence Tumpey’s team at the US Department of Agriculture’s poultry research lab in Athens, Georgia, got quite different results: they found that mice given oseltamivir still got sick and 1 in 10 died. It is not clear why Kawaoka’s mice fared better.
What is more, all the safety precautions are aimed at preventing escape, not dealing with it should it occur. If any of Kawaoka’s lab workers are exposed to the virus despite all the precautions, and become infected despite taking oseltamivir, the consequences could be disastrous.
“I experienced disbelief…regarding the decision to relocate the reconstructed 1918 influenza strain from a BSL-4 facility to a BSL-3 facility, based on its susceptibility to antiviral medication,” Ronald Voorhees, chief medical officer at the New Mexico Department of Health, wrote on ProMED-mail, an infectious diseases mailing list.
Yet Kawaoka’s decision does comply with the US National Institutes of Health guidelines for BSL-3 agents: those causing “serious or lethal human disease for which preventive or therapeutic interventions may be available”. In fact, he is considered unusually cautious. “Kawaoka should be applauded for using BSL-4 at all,” says Richard Webby, a flu researcher at St Jude’s Children’s Hospital in Memphis, Tennessee.
Exposing monkeys
By contrast, the team in Georgia, the first to experiment with genetically engineered 1918 viruses, did all its work at BSL-3Ag. Meanwhile, Michael Katze at the University of Washington at Seattle is planning to expose monkeys to aerosols of 1918-type viruses at BSL-3, a step down from BSL-3Ag. The recent SARS escapes were from BSL-3 labs.
“We would have to do any such work at BSL-4,” says John Wood of the UK’s National Institute for Biological Standards and Control. In the US, the differing standards applied by different groups are due to the fact that experiments on engineered viruses such as the 1918 flu are approved on a case-by-case basis by Institutional Biosafety Committees (IBCs), composed of local scientists and officials. Critics say these are free to interpret the official guidelines in a way that suits them.
“There is no effective national system to ensure consistency, responsibility and good judgement in such research,” says Edward Hammond of the Sunshine Project, a biosecurity pressure group in Austin, Texas. In a review of IBCs published this month, he found that many would not provide minutes of recent meetings as required by law.
He says the IBC that approved the planned 1918 flu study at the University of Washington considered only one scenario that could result in workers being exposed to airborne virus – the dropping of samples. Its solution: lab workers “will be trained to stop breathing”.

